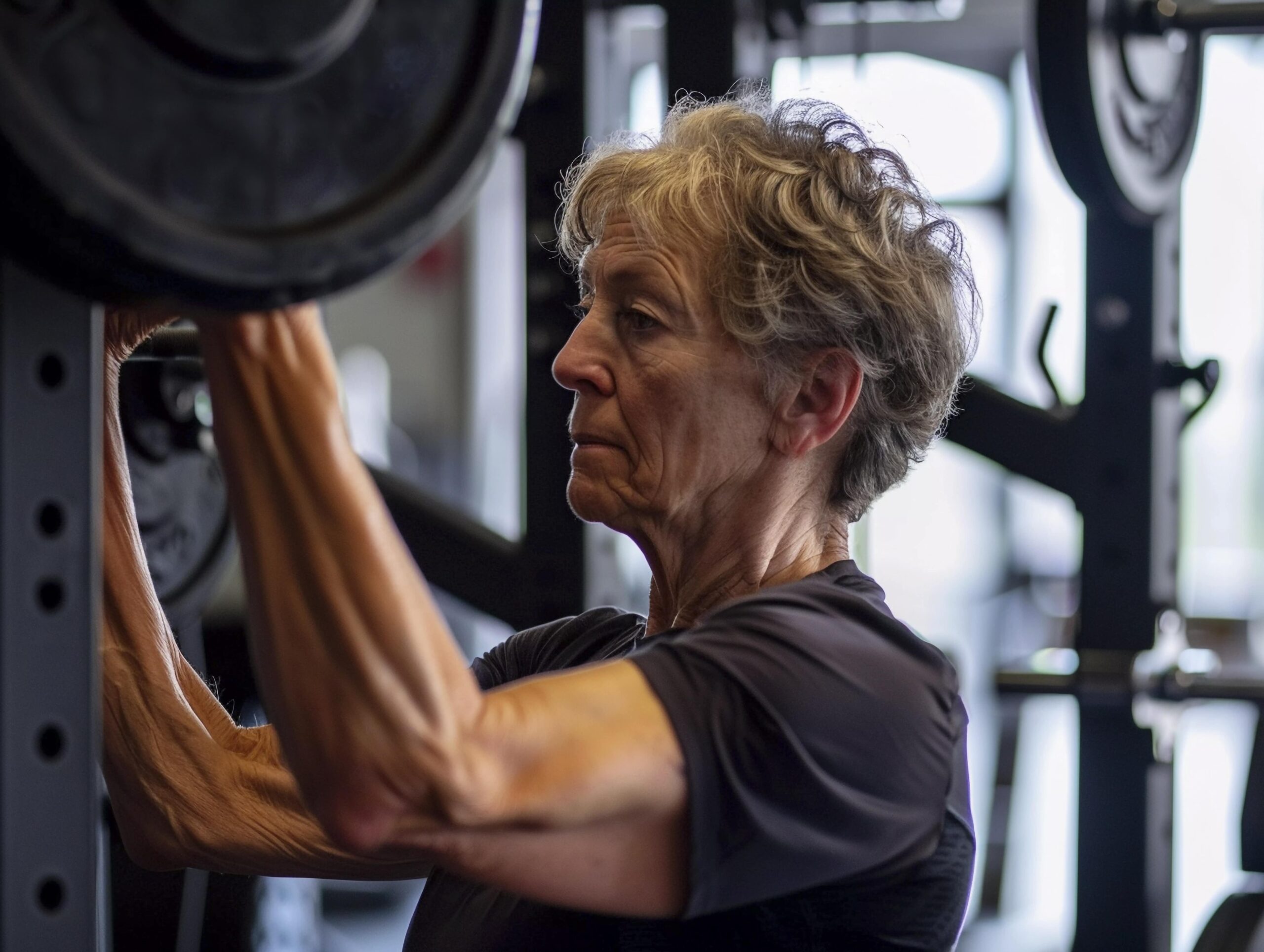Menopause and Weight Gain—Why Does It Happen?
Weight gain during menopause is a common concern—and it’s not just about calories. It’s the result of a complex mix of hormonal shifts, lifestyle factors, and changes in metabolism.
Hormones & Fat Distribution
Estrogen levels decline during menopause, which affects how and where your body stores fat—especially around the waist, known as “menopause belly.” Lower estrogen also impacts hunger and fullness cues, making cravings harder to resist.
Sleep, Stress & Metabolism
Sleep often takes a hit during menopause, which disrupts appetite-regulating hormones and raises stress levels—both of which can lead to weight gain. Add in a slower metabolism and changing body composition, and it becomes harder to shed extra kilos.
Health Matters
Menopausal weight gain isn’t just cosmetic. It increases the risk of heart disease, diabetes, and worsens symptoms like hot flushes and joint pain.
What Can Help?
Movement That Matters
- Strength training helps maintain muscle and bone strength.
- Cardio (like walking, cycling, HIIT) supports heart health and fat loss.
- Yoga or Pilates improves flexibility, posture, and mental well-being.
Nourish, Don’t Restrict
- Focus on whole foods—veggies, whole grains, lean protein, and healthy fats.
- Add phytoestrogen-rich foods (soy, flaxseeds, chickpeas) for hormonal support.
Consider HRT
- Hormone therapy may support weight management by improving sleep, mood, and energy levels—though its impact on fat loss varies. Always discuss it with your doctor.
Prioritise Sleep & Stress Care
- Good sleep and mindfulness practices (like CBT, breathwork, or yoga) can regulate hormones and improve your emotional well-being.
Ready to take control?
Our expert team—specialists, dietitians, and lifestyle coaches—can help create a personalized, holistic plan to manage weight during menopause. Book your consultation today and feel empowered to thrive in midlife and beyond.